Find Out About
Pericoronitis
Pericoronitis is a wisdom tooth infection of the gum around a wisdom tooth. Infection gets into the gum because the tooth has not grown all the way through, and there is a flap of gum tissue over the top of the tooth.
 flap of gum over a tooth
flap of gum over a toothBacteria in saliva can get under the gum flap, and set up an infection.
How does this happen? As the wisdom tooth grows under the gum, it pushes up on the gum from underneath. The gum gets thinner and thinner as the tooth slowly moves up over a period of months. But the gum is still intact over the tooth, and so bacteria cannot get under the gum. But at some point, one of the cusps of the tooth breaks through the gum.
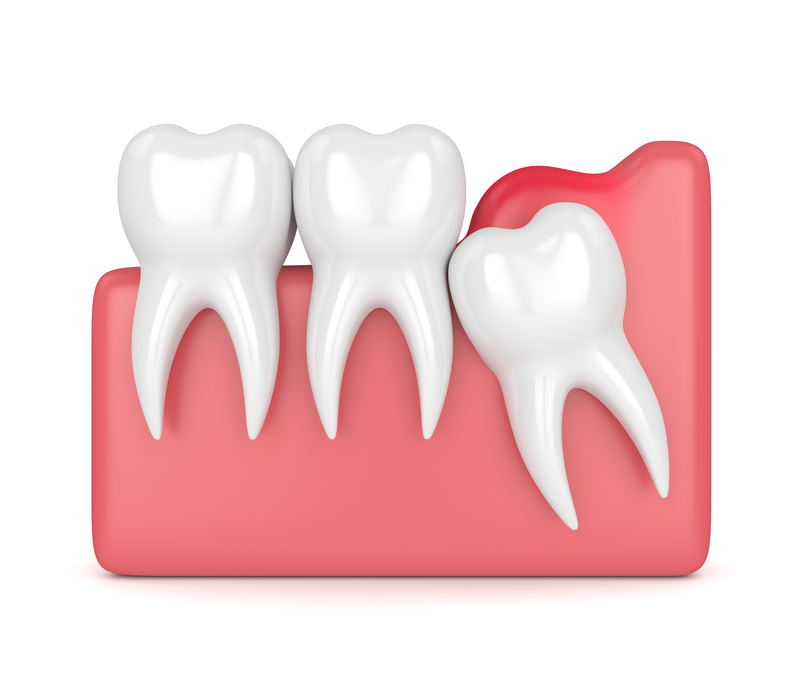 wisdom tooth just breaking through the gum
wisdom tooth just breaking through the gumFrom now on, the tooth is no longer sealed off from the bacteria in your saliva. The bacteria can get under the gum, and set up a little colony right there. These are bacteria that are normally present in everybody's mouth, they are not some kind of new infection!
But problems can start because the bacteria can hide under the flap of gum that is still covering most of the top of the wisdom tooth. This means they are not exposed to the normal flow of saliva, and are in a low-oxygen situation.
Bacteria that can grow without oxygen are called "anaerobic" bacteria. While we all have them in our mouths to some degree, they are kept in check by the oxygen in our saliva.
But when they get into a low-oxygen situation, like under the flap of gum covering a wisdom tooth, they can multiply rapidly, and set up an infection.
Pericoronitis
What are the symptoms of pericoronitis?
What does it feel like?
Pericoronitis symptoms start with a sore gum. It feels like the gum at the back of mouth, just behind a back tooth, is sore. At the start, it feels like you maybe scratched the gum with a peanut or something like that. When it goes on for a few days, you can feel that the gum at the back is getting slightly swollen.
As the infection spreads, you might start to feel that it's harder to open your mouth normally. It's partly because your jaw feels "stiff" to open, and partly because it's painful if you try to open your mouth any wider.
To make things worse, it's not unusual to get pain when you try to bring your teeth together. This is caused by the upper wisdom tooth hitting the gum over the lower wisdom tooth.
What does it look like?
It can be hard to see all the way to the back of your mouth, but if you get a good light, you may be able to see that the gum behind the last tooth is red and swollen. If the top tooth is hitting the lower gum, you can even see some "dents" in the gum, which are the imprint of the upper tooth.
Remember to check out my top recommended electric toothbrush, which has the best performance and a great price at Amazon - the Cybersonic 3 brush.
What can you do about pericoronitis?
There are a couple of things that can be done.
- Aloe vera gel. This is surprisingly effective - but you need to use a high-quality gel to get the benefits. The best is from Forever Living. You just put a small blob of the gel on your fingertip, and then rub it gently over the painful area of gum, over the wisdom tooth.
The antiseptic and anti-inflammatory
properties of the aloe gel will kill the bacteria under the gum flap,
and reduce the swelling, making things much more comfortable. You will
need to re-apply the gel every hour or so at first, until the swelling
goes down.
- Mouthwashes. The simplest (and cheapest) is to rinse around the affected gum with really hot salty water. The heat opens up the blood capillaries and helps your own immune system to swing into action. The physical effect of swishing around vigorously can wash out the build-up of bacteria from under the gum. And the bacteria don't like the salt. But you have to do this every hour through the day, for 2 to 3 days.
A more effective solution is a mouthwash that releases oxygen, to kill the low-oxygen-loving bacteria. This works better than hot salt water alone, providing you keep the mouthwash in your mouth for long enough. AND you have to swish it forcefully around the inflamed gum to get enough of the oxygen-releasing mouthwash in the right spot.
I recommend a high-quality peroxide-containing mouthwash. The BEST one is the TheraBreath Oral Rinse, available from Amazon.
ALSO
- Syringing mouthwash under the gum flap. If you have a small plastic syringe, it may be possible to direct a jet of hot salt water or oxygen-releasing mouthwash right under the gum flap. If you are a ble to do this, it can be very effective.
But first you need to have a small plastic syringe to hand. And you need to be able to get it to the back of your mouth. And then you have to be able to get the tip just at the edge of the gum flap. Not easy!
- Antibiotics. When the infection has progressed far enough to cause you difficulty opening your mouth, or you have a raised temperature, it's time for some antibiotics. Obviously, then best one will be an antibiotic that works on "anaerobic" bacteria.
The commonest one is Metronidazole ("Flagyl"), but you must avoid alcohol while you are taking these tablets. The usual dose is 200mg every eight hours, but this may depend on the severity of the infection.
- Removal of the opposite tooth. Surprisingly, for pericoronitis over a lower wisdom tooth, sometimes the quickest relief can be obtained by removing the upper wisdom tooth. This is because the upper tooth sometimes grows down enough to start biting on the gum over the lower tooth, causing trauma to the gum.
When you add a gum infection like pericoronitis to the situation, the lower gum swells up, and gets hit by the upper tooth even more! Removing the upper tooth (normally a simple procedure) instantly eliminates the trauma to the gum, and the pain relief can be significant.
- Removal of the wisdom tooth, infection allowing. The most obvious solution is to remove the offending tooth itself, but this isn't always possible straightaway. If you can't open your mouth very wide, it's awkward for the dentist to reach all the way back there. (Whereas for an upper wisdom tooth, removal can be done with your mouth pretty much closed!).
Also, we don't like removing a tooth that has an active infection around it, due to the risk of spreading the infection. So mouthwashes and antibiotics first, then wisdom tooth removal later.
BUT it's not always necessary to remove the wisdom tooth. If the pericoronitis is due to a short-term infection as the tooth comes through, and it has enough room to grow into position properly, then we just deal with the infection as simply as possible, and give the tooth a chance to reach it's final position.
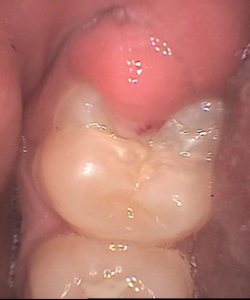
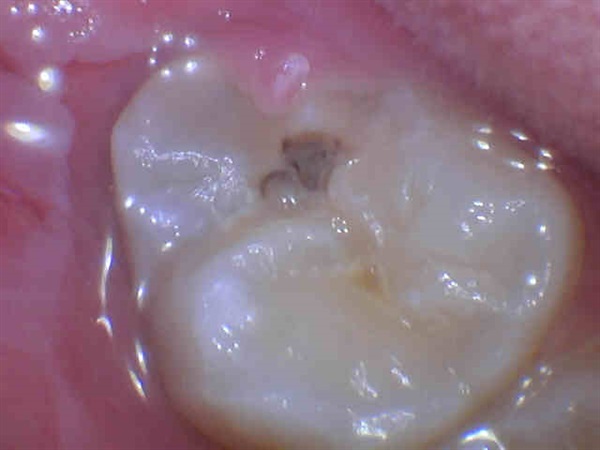 pericoronitis behind a wisdom tooth
pericoronitis behind a wisdom toothIn the image above, the tooth has almost grown into its final position. The flap of gum has become smaller. Now there's just that small cavity to deal with!
While most gum infections are just uncomfortable rather than anything more, pericoronitis can progress to become much more serious, interfering with mouth opening and even swallowing. You should always take any wisdom tooth infection seriously.
Get to a dentist as soon as you can!
You may also find this page useful; Tooth Abscess Antibiotics