Lyme Disease Blood Test
A single Lyme disease blood test does not always show that you have the bacteria responsible for causing Lyme disease in your body.
In fact, the standard preliminary Lyme disease blood test most often used to screen for the presence of the Lyme bacteria (Borrelia Burgdorferi) can FAIL to pick up the bacteria in about 50% of tests.
That means that it only shows a positive result HALF the time when Lyme bacteria are present!
WHY would anybody use a test that only works half the time?
Pretty much because it's "the way it's always been done", and medical insurance companies will pay for the test. Doctors will always try to make the diagnosis of Lyme disease based on the symptoms that the patient has, and on a physical exam of the patient, to start off with.
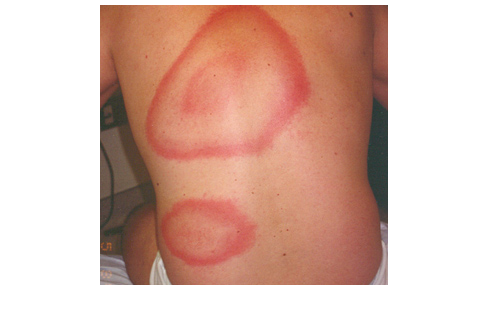 bullseye target lesion
bullseye target lesionBut they can't make a 100% CERTAIN DIAGNOSIS of Lyme disease without blood tests.
Sometimes a patient will turn up who has clinical symptoms that are similar to Lyme disease, but they cannot recall if they were bitten by a tick or not. In those instances, it will be necessary for blood tests to determine the cause of the patient's symptoms, and to rule out Lyme disease.
The most commonly accepted INITIAL SCREENING Lyme disease blood test is called the ELISA test. ELISA stands for enzyme-linked immunosorbent assay.
BUT the ELISA does NOT test for the Lyme bacteria itself - it looks for the cells that the human body creates to try and fight the bacteria - This screening test actually looks for the antibodies that the human body makes in response to the causative bacteria Borrelia Burgdorferi.
When the human immune system is "challenged" by a specific bacteria, it begins to produce antibodies to try and kill that foreign bacteria. This is how your immune system works.
These antibodies that your immune system creates are specific for the bacteria that triggers the immune response. They are unique. They only work against that one type of bacteria.
These specific antibodies can be detected using the ELISA test.
SO, if the ELISA test shows that you have the antibodies against the Borrelia bacteria, the ONLY WAY you could have them is if you have the Borellia bacteria in your system!
BUT THERE'S A PROBLEM
The ELISA test is only 50% reliable in detecting your immune system's response to Lyme bacteria. Especially during the early stages of the infection, but also in long-term "chronic" Lyme infections, the test may not show up as positive, even though the bacteria are growing in your system.
Lyme Disease Blood Test
However, if there are other clinical symptoms of Lyme disease, your doctor may well make the assumption that you DO have Lyme disease, and start to treat you, while he waits for a subsequent ELISA test to show positive.
For information on the symptoms of Lyme Disease, go to Symptoms Lyme Disease.
If you DO get a positive result from the ELISA Lyme disease blood test, another different test is needed. This is called a Western blot test.
The Western Blot test CONFIRMS that there are actual antibodies to the Borrelia Burgdorferi bacteria.
The Western Blot method is more complicated than the ELISA test. It involves separating the sample into its component proteins using an electrical current. Then, these proteins are transferred to a special kind of blotting paper and reacted with your blood sample. An enzyme is used to cause color changes.
Testing laboratories performing a Western Blot test use an electrical current to separate proteins called antigens into bands. The read-out looks something like a bar code. The laboratory compares the patterns produced from YOUR blood sample to a standard pattern in a known case of Lyme disease. If your test result shows the right number of bands that match the "standard" bands, YOU HAVE A positive result.
Most Lyme disease blood test authorities say that at least 5 out of the 10 bands must match for a positive test result. BUT, because some bands on the Western Blot are more significant than others, your doctor might conclude that you DO have Lyme, even if your Western Blot test does not have the band matching recommended.
Different testing laboratories use different methods and criteria for interpreting the test. It is theoretically possible to get a positive result from one lab, and a negative test result from another!
BECAUSE the Western Blot is more sensitive than the ELISA test, some authorities recommend skipping the ELISA when there is a suspicion of Lyme disease. They recommend going STRAIGHT to the Western Blot, to save time and expense.
OTHER LYME DISEASE BLOOD TESTS
There are 3 other tests that can be used to detect Lyme disease.
- Polymerase Chain Reaction (PCR)
- Antigen Detection
- Culture Testing
- These tests are called DIRECT TESTS because they detect the ACTUAL bacteria, not just your body's immune system reaction to it.
PCR multiplies a key portion of DNA from the Lyme bacteria so that it can be detected. While PCR is highly accurate when the Lyme DNA is detected, it can produce "false negatives". This is because Lyme bacteria are thinly distributed in the blood, and so there may not be any Lyme bacteria in the blood sample tested
Antigen detection tests look for a unique Lyme disease protein in a body fluid, such as urine or synovial (joint) fluid. Some patients who get NEGATIVE results with other initial screening tests prove positive on this test.
Culture Testing is THE BEST TEST for identifying Lyme bacteria. The testing laboratory takes a sample of blood or other fluid from the patient, and tries to grow the Lyme spirochetes in a special growth medium. Although culture tests are generally accepted as proof of infection, this type of test is relatively NEW, and needs more development. This is particularly important, when we think about the generally LOW QUALITY of the traditional Lyme disease blood test currently in use.
After confirmation of diagnosis, treatment is the next step.
For some information on Lyme Disease treatment, have a look at How to treat Lyme Disease.
Doctors may also wish to check other routine laboratory tests to determine how severely the patient's body has been affected by the Lyme disease. Other blood tests include:
White Blood Cell Count
Sedimentary Rate.
These tests are helpful to determine if the bacteria has spread throughout the body. Testing of synovial fluid and cerebro-spinal fluid may be needed if the patient presents with Lyme disease induced arthritis or Lyme disease induced meningitis.